Vitamin C (ascorbic acid), is an essential water-soluble nutrient, which humans need on a daily basis. It is widely accepted by the European Food Standards Agency (EFSA) and other academic bodies that Vitamin C contributes to the normal function of the immune system but other substances in fruit such as citrus bioflavonoids also have important properties.

Sources of Vitamin C and Citrus Bioflavonoids
Vitamin C cannot be made, in the body as we lack the enzyme L-gulonolactone oxidase required for ascorbic acid synthesis. It only it lasts for a short period of time in the blood stream so it needs to be ingested regularly every day. Likewise the common citrus bioflavonoids such as hesperidin, naringin, tangeretin and quercetin have to be ingested regularly. Vitamin C is commonly available in citrus fruits, berries, vegetables and nuts and the citrus bioflavonoids are found in the in the pulp and white core that runs through the centre of lemons, limes, oranges, pomegranates, green peppers, cherries, and grapes. Although these foods are commonly available, in view of their daily requirements, some Western type diets have days were intake is inadequate so extra supplementation would be helpful. Most only contain vitamin C so it’s important to take a supplement which also contains the important citrus bioflavonoids.
Biochemical roles in the body

Vitamin C is often described as an antioxidant, but this is not actually correct. It does not have direct free radical neutralising effects like vitamin E and vitamin A. There are concerns with taking supplements containing vitamin A and vitamin E as the may mop up too many free radical (some of which are needed for the normal function of the cell). This concern does not relate to vitamin C even in relatively higher doses. More specifically, Vitamin C is involved in the mechanism that enables DNA to ‘sense’ the oxidative damage done by free radicals produced viral and bacterial infection, toxic chemicals, inflammation by integrating with the iron imbedded in DNA. This process facilitates repair of the DNA damage caused by oxidative damage and is therefore a significant aspect of immune function. Vitamin C may also have cancer protective properties by limiting the formation of carcinogens, such as nitrosamines from meat and instead converts them into Nitric oxide (NO) which is linked to lower blood pressure, better tissues oxygenation and improved sports performance. Vitamin C has also been shown to protect intracellular components from toxic products such as hydrogen peroxide via inhibition of gap-junction intercellular communication. Finally vitamin C is a cofactor for several enzymes and plays an important role in the synthesis of collagen and cellular defence apparatus.
This protection is needed every minute of every day as, according to estimates, each cell in the body can be expected to experience approximately 100,000 potentially DNA-damaging events daily. So a healthy DNA repair system is imperative.
General benefits of polyphenols: The multiple benefits of polyphenols (including bioflavonoids) have been described in detail elsewhere but in a nutshell includes; feeding health bacteria in the gut, improving gut health, reducing excess chronic inflammation, enhancing antioxidant enzymes and protecting joints – read more
Vitamin C deficiency
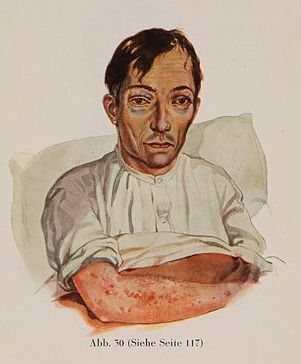
In today’s society scurvy is rare, although can still be found amoung elderly people in social isolation or those with mental illness, especially if they smoke heavily. More relevant is health implications of having chronically low levels which as been linked with an increased risk of a important degenerative conditions such as high blood pressure, macular degeneration, gallbladder disease, atherosclerosis, heart attacks and stroke. Higher than normal levels, especially produced through intravenous ascorbic acid, have not been shown to reduce the incidence of these disease.
The recommended daily amount of vitamin C are based on its known physiological and antioxidant functions in white blood cells and are probably much higher than the amount required for protection from deficiency in adults this is between 80-100mg /day. Men need 10% more than women until they pregnant or lactating when the RDA is around 120mg/day. Smokers should take another 35% (around 120-140 mg/day). Normal blood levels are between 34-114 micromols/l.
Dietary fruit, vitamin C and citrus bioflavonoids

Fruit juices and smoothies: These are a reasonable way to increase your fruit intake but they also increase the effect of the sugar by speeding up how quickly it is absorbed into the blood stream (glycaemic index). Eating excess sugar and other high glycemic index food have significant health concerns. Most juice and smoothie aficionados mix them with plenty of vegetables but an increasingly used and sensible phrase used in healthier circles is; “Eat your fruit and juice your vegetables”
If you do make fruit juices, ideally they should be drunk fresh. After squeezing, juice changes its chemical composition quickly becoming more acidic and losing its nutritional content. Juices within cartons have generally been heavily processed increasing their sugar content and often need the vitamin C re-added to keep the levels up. Many also have added extra sugar and these should definitely be avoided. Despite the drawn back of juices they are still a better alternative than sugary canned drinks so on a hot summer day consider a freshly squeezed orange mixed, mint, water and ice which may entice kids to more a healthier option. One lemon squeezed into a pitcher with a spoon of honey topped up with sparkling water makes healthier lemonade for children.
Fruit intake, indigestion and the alkaline diet: People often say – “I can’t eat fruit because I have indigestion or heartburn”. Although it is true that initially fruit can result in a little irritation in vulnerable individuals, it is not the root cause of the problem and in the long term fruit will improve the health of the stomach and oesophagus (gullet). The underlying cause is usually an unhealthy balance of fat, meats and sugar which the stomach has to work harder to digest – i.e. produce more of its own hydrochloric acid. To make matters worse, sufferers often turn to antacids for immediate relief. The stomach then senses a more alkaline environment and responds by producing yet more acid, perpetuating the problem. On the other hand, consumption of mildly acidic fruit sends signals to the stomach lining to produce less of its own acid. After a while, with perseverance, eating fruit and other less gastric-irritating foods will therefore reduce the acid levels (make the stomach more alkaline) and improve the health of gastric lining, and thus prevent indigestion.
Vitamin C and cancer prevention
Most case-control studies and epidemiologic evidence suggests that higher consumption of fruits and vegetables is associated with lower risk of most types of cancer including lung, breast, colon or rectum, stomach, oral cavity, larynx or pharynx, and esophagus. This may, in part, due to their high vitamin C content although fruit also contains other healthy components including fibre, other vitamins, minerals and polyphenols.
Evidence from prospective cohort studies is compounded by the issue that people who eat more fruit are generally more health conscious, less likely to smoke, be overweight and more likely to exercise. The other elements of fruit such as the fibre and citrus bioflavonoids are also healthy independent on the vitamin C content. There are some studies which large enough for the statistician to exclude these other influences in the statistical analysis. For example in the massive Nurses’ Health Study, consumption of an >200 mg/day of vitamin C from food compared with < 70 mg/day was associated with a lower risk of breast cancer especially premenopausal women with a family history. On the other hand, two other large cohort trial found no increase in cancer if individuals consumed over 87mg/day and certainly no reduction if they consumed over 200mg/day. It appears, from this data that taking over the required amount of vitamin C does not reduce cancer risk but being deficient does increase the risk.
Most randomized controlled studies, investigating the potential anti-cancer properties of vitamin C supplements have combined them other micronutrients. For example, in the Supplémentation en Vitamines et Minéraux Antioxydants (SU.VI.MAX) study, a randomized, double-blind, placebo-controlled clinical trial, 13,017 healthy French adults received supplementation with 120 mg ascorbic acid, 30 mg vitamin E, 6 mg beta-carotene, 100 mcg selenium, and 20 mg zinc, or placebo. After a median follow-up time of 7.5 years, men, in the supplementation group had lowered total cancer incidence. Further analysis of dietary habits of men in the study relieved many had inadequate intake of these nutrients and they like explanation for the benefit and the supplement restored the level to the normal range.
In the Physicians’ Health Study II, supplements containing 500 mg/day vitamin C plus 400 IU vitamin E every other day for a mean follow-up period of 8 years failed to reduce the risk of prostate or total cancer compared with placebo in middle-aged and older men participating. Similar findings were reported in women participating in the Women’s Antioxidant Cardiovascular Study. Compared with placebo, supplementation with vitamin C (500 mg/day) for an average of 9.4 years had no significant effect on total cancer incidence or cancer mortality. Likewise, in a large intervention trial conducted in Linxian, China, daily supplements of vitamin C (120 mg) plus molybdenum (30 mcg) for 5–6 years did not significantly affect the risk of developing esophageal or gastric cancer.
A 2008 review of vitamin C, beta-carotene, vitamin A, or vitamin E found no convincing evidence that vitamin C (or) prevents gastrointestinal cancers. A similar review by Coulter and colleagues found that vitamin C supplementation, in combination with vitamin E, had no significant effect on death risk due to cancer in healthy individuals.
A substantial limitation in interpreting many of these studies is that investigators did not measure vitamin C concentrations before or after supplementation. Plasma and tissue concentrations of vitamin C are tightly controlled in humans. At daily intakes of 100 mg or higher, cells appear to be saturated and at intakes of at least 200 mg, plasma concentrations increase only marginally. If subjects’ vitamin C levels were already close to saturation at study entry, supplementation would be expected to have made little or no difference on measured outcomes – on the other hand if they were low they may well have helped.
The evidence for high dose vitamin C

In the 1970s a Scottish surgeon, Ewan Cameron, his colleague, Allan Campbell and chemist Linus Pauling worked on the potential links between vitamin C and cancer. It is often misquoted that this reserach won a Nobel prize. This is incorrect; Professor Pauling won a Nobel prize in 1954 for his work on chemical bonds winning, 25 years earlier. The team conducted two clinical trials in which 50 advanced-cancer patients were treated with large doses of oral vitamin c. Patients received intravenous (IV) ascorbic acid (10 g /day for 10 consecutive days; some patients received higher doses), oral ascorbic acid (10 g/day), or both. The subjects exhibited a wide variety of responses to treatment, however, the lack of controls prevented definitive assignment of any beneficial responses to the ascorbic acid treatment.
In 1975, a published case report of a single patients reported improvement in well-being and resolution of lung masses after being treated with IV ascorbic acid. When the patient’s daily dose of ascorbic acid was reduced, some of signs of the disease returned; however, remission was temporarily achieved again after the patient reverted to the higher initial dose. In 1976 a 100 patients with terminal cancer were treated with oral ascorbate (10 g/day for 10 days IV, then orally) were compared with non-randomised matched controls from the same hospital and reported better survival rates of around 300 days.
In 1979 and 1985 the first randomized placebo controlled trials were conducted but used either 10 g or oral vitamin C or placebo daily until signs of cancer progression. At the end of each study, no significant differences were noted for symptoms, performance status, or survival.
In 2006 a further three case reports were published involving IV Vit-C amoung terminal cancer patients who received between 15 g to 65 g, IV initially once or twice a week for several months. Patients also used additional treatments, including other vitamins vitamins, minerals, and botanicals. The authors felt survival was longer than expected but there were no controls to compare with.
In 2007 and 2011, two non randomized studies demonstrated that IV vitamin C treatment resulted in improved quality of life and decreases in cancer-related side effects in cancer patients but again their were no controls to compare with. Other trials have combined vitamin C with chemotherapy with reported improvements in toxicity but as no disease outcomes were used we do not know whether vitamin C just reduced the effect of chemotherapy.
Conclusion:
Inadequate levels of vitamin C should be avoided as low levels are linked to a higher risk of degenerative diseases including cancer. Only small amounts of vitamin C are required to avoid scurvy but significant higher avoids are likely to be needed to ensure the cellular protection and immune support properties. Although trials have shown that taking oral supplements even at relatively high doses (over 100mg) does not do any harm, these levels have not been shown to reduce cancer risks compared to those with adequate levels. No randomised trial has compared high-dose intravenous Vitamin C with placebo within a statistically robust design. A trial is needed to solve the IV vitamin C dilemma although this lack of data has not stopped many nutritional therapist promoting high dose IV vitamin in their routine practice.
The influence of citrus bioflavonoids has previously been underestimated and it’s very important to get adequate intake of this important polyphenols either with daily high fruit, vegetable intake or if necessary a supplement which contains them. The potential anti-viral properties, particularly of the bioflavonoids, has drawn the attention of the covid-19 research committees for further investigation, along side other foods but there is no current evidence for an effect. Nevertheless, in view of its proven immune support properties, ensuring adequate levels of both vitamin C and citrus bioflavonoids in this current crisis seems very sensible.
.
References for Vitamin C and Citrus Bioflavonoids :
Cameron E, Campbell A: The orthomolecular treatment of cancer. Clinical trial of high-dose ascorbic acid in advanced human cancer. Chem Biol Interact 9 (4): 285-315, 1974
Cameron E et al: Reticulum cell sarcoma: double complete regression induced by high-dose ascorbic acid therapy. Chem Biol Interact 11 (5): 387-93, 1975.
Cameron E, Pauling L: Ascorbate in the supportive treatment of cancer: Prolongation of survival times in terminal human cancer. Proc Natl Acad Sci 73 (10): 3685-9, 1976
Cameron E, Pauling L: Supplemental ascorbate in the treatment of cancer: prolongation of survival times in terminal human cancer. Proc Natl Acad Sci 75 (9): 4538-42, 1978.
Creagan ET et al.: Failure of high-dose vitamin C therapy to benefit patients with advanced cancer. A controlled trial. N Engl J Med 301 (13): 687-90, 1979
Moertel CG, et al.: High-dose vitamin C versus placebo in patients with advanced cancer who have had no prior chemotherapy. RCT. N Engl J Med 312 (3): 137-41, 1985.
Padayatty SJ et al.: Intravenously administered vitamin C as cancer therapy: three cases. CMAJ 174 (7): 937-42, 2006.
Vollbracht C et al.: Intravenous vitamin C administration improves quality of life in breast cancer patients during chemo-/radiotherapy and aftercare: results of a retrospective, multicentre, epidemiological cohort study In Vivo 25 (6): 983-90, 2011.
Yeom CH et al: Changes of terminal cancer patients’ health-related quality of life after high dose vitamin C administration. J Korean Med Sci 22 (1): 7-11, 2007.
Padayatty SJ: Vitamin C pharmacokinetics: implications for oral and intravenous use. Ann Intern Med 140 (7): 533-7, 2004.
Uchide N, Toyoda H Antioxidant therapy as a potential approach to severe influenza-associated complications. Molecules. 2011. 28; 16(3):2032-52.
Ge H, Wang YF, Xu J, Anti-influenza agents from Traditional Chinese Medicine.
Nat Prod Rep. 2010; 27(12):1758-80.
Li SY, Chen C, Zhang HQ, Guo HY, Wang H, Wang L, et al. Identification of natural compounds with antiviral activities against SARS-associated coronavirus. Antivir Res. 2005;67:18–23
Yang ZF, Bai LP, Huang WB et al. Comparison of in vitro antiviral activity of tea polyphenols against influenza A and B viruses and structure-activity relationship analysis. Fitoterapia. 2014; 93:47-53
Lin CW, Tsai FJ, Tsai CH, Lai CC, Wan L, Ho TY, et al. Anti-SARS coronavirus 3C-like protease effects of plant-derived phenolic compounds. Antivir Res. 2005;68:36–42.
Yu MS, Lee J, Lee JM, Kim Y, Chin YW, Jee JG, et al. Identification of myricetin and scutellarein as novel chemical inhibitors of the SARS coronavirus helicase, nsP13. Bioorg Med Chem Lett. 2012;22:4049–54.
Lau KM, Lee KM, Koon CM, Cheung CS, Lau CP, Ho HM, et al. Immunomodulatory and anti-SARS activities of Houttuynia cordata. J Ethnopharmacol. 2008;118:79–85.
World Health Organization. [Last accessed on 2020, 1.4.2020]. Available from: http://www.who.int .
Wu W, Li R, Xianglian Li X, et al Quercetin as an Antiviral Agent Inhibits Influenza A Virus (IAV) Entry. Viruses. 2016 Jan; 8(1): 6.
Song J, Park K, Kwon D et al Anti-human rhinovirus 2 activity and mode of action of quercetin-7-glucoside from Lagerstroemia speciosa. J Med Food. 2013 Apr;16(4):274-9. doi: 10.1089/jmf.2012.2290.
Ryu YB, Jeong HJ, Kim JH, et al. Biflavonoids displaying SARS-CoV 3CL (pro) inhibition. Bioorg Med Chem. 2010;18:7940–7.
Hoffer LJ: Phase I clinical trial of i.v. ascorbic acid in advanced malignancy. Ann Oncol 19 (11): 1969-7
Lin L, Hsu W, Lin C et al Antiviral Natural Products and Herbal Medicines J Tradit Complement Med. 2014 Jan-Mar; 4(1): 24–35. doi: 10.4103/2225-4110.124335
Mycol V., Kotwal G.J., Longum P. Natural Antivirals against Human Viruses with Bitter melon. Virol. Mycol. 2014;3:3–5.
Paredes A1, Alzuru M, Mendez J et al Anti-Sindbis activity of flavanones hesperetin and naringenin. Biol Pharm Bull. 2003;26(1):108-9.
Kotwal G. Natural anti-virals against human viruses, Virol Mycol 2014, 3:2 DOI: 10.4172/2161-0517.1000e107
Neurath AR, Strick N, Li YY, Debnath AK (2004) Punicagranatum (Pomegranate) juice provides an HIV-1 entry inhibitor and candidate topical microbicide. BMC Infect Dis 4: 41.
Su X, Sangster MY, D’Souza DH (2010) In vitro effects of pomegranate juice and pomegranate polyphenols on foodborne viral surrogates. Foodborne Pathog Dis 7: 1473-1479.
Kaul TN, Middleton E Jr, Ogra P et al Antiviral effect of flavonoids on human viruses. J Med Virol. 1985, 15(1):71-9.